What Is a Tracheostomy?
A tracheostomy is a surgically made opening (called a stoma) in the front of the neck that goes directly into the airway (trachea). A tracheostomy (tray-kee-OSS-tuh-me) tube, or trach tube, keeps the pathway open so air can go through the tube, into the airway, and to the lungs.
The word trach (say: "trake") can refer to the procedure, the opening, or the tube itself.
Why Are Tracheostomies Done?
Doctors might do a tracheostomy (also called a tracheotomy) if a child:
- has a blocked airway and air can’t get to the lungs by breathing through the nose or mouth
- can't clear secretions (mucus in the airway) from the airway on their own
- needs to be on a ventilator for an extended time
Trachs can stay in place for a long time, if needed.
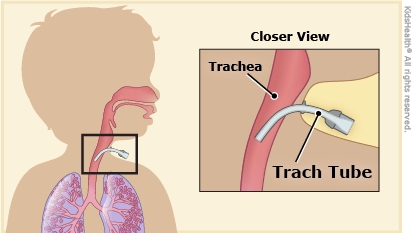
What Happens During a Tracheostomy?
A child getting a tracheostomy will get general anesthesia to sleep through it and not feel pain. In the operating room, the surgeon will:
- Make an incision into the skin of the neck.
- Make a small hole (the stoma) in the trachea near the base of the neck.
- Insert the trach tube through the stoma to keep the pathway open so air can move to and from the lungs.
- Attach ties to the front part of the trach tube to keep it from slipping out of the hole.
A trach tube might be permanent, but some can be removed later if a child no longer needs it.
How Can Parents Help?
To help prevent infection and other problems, the care team will teach you:
- how to clean the area around the trach tube
- how to change the trach ties
- when and how to change the tube
Trach tubes sometimes can get blocked with thick mucus. If this happens, it’s hard for a child to get enough air into the airway during breathing. The care team will show you how to use a suction machine to clear mucus from the trach tube. Regular suctioning and taking steps to thin the mucus can help prevent a blockage.
When caring for the tube:
- Always wash your hands before and after caring for your child's trach tube or stoma.
- Clean the opening around the tube as instructed by the care team.
- Follow the schedule from the care team for suctioning the tube, changing the trach ties, and replacing the tube.
- Keep sprays, powders, perfumes, pet hair, and sand away from your child’s trach tube.
- Keep water out of the trach.
- Use a heated humidifier and/or heat-moisture exchanger (HME) with your child's trach tube as instructed by your care team.
What Else Should I Know?
Kids may need to learn new ways to speak with a trach tube in place. Ask the care team if a speech therapist could help your child. Having a tracheostomy usually doesn’t affect eating and drinking, but if it does, a speech therapist also can help with this.
Always have a bag of supplies with your child in case the trach tube gets clogged with mucus or comes out. Your child should always have someone with them who is trained to handle emergencies.
When Should I Call the Doctor?
Call the doctor if the area around the tube is bleeding, or if your child:
- is in pain
- has warmth, swelling, or redness around the stoma
- has a fever
- has a cough
- has foul-smelling, thick, or blood-streaked mucus; a change in color of the mucus; or a lot of mucus in the tube
- needs more oxygen than usual
- has a drop in oxygen levels (called desaturation)
- is very tired or seems anxious
- throws up or has trouble with feeding
If the tube comes out, reposition it as the care team taught you. If you can’t get it back in place, insert a new tube as you were shown.
Call 911 right away if you can’t get a trach tube into place. Also call if:
- Your child has a desaturation that does not improve with the steps the care team taught you.
- Your child is not breathing or has trouble breathing.
- Your child's lips or skin look blue or gray.
- There's bright red bloody mucus in the trach.



