Hydroxyurea for People With Sickle Cell Disease
What Is Hydroxyurea?
Hydroxyurea is a medicine that can help people who have sickle cell disease. It keeps blood cells round and flexible, so they flow better and deliver oxygen to the body more easily. This means less pain and fewer trips to the hospital.
What Happens in Sickle Cell Disease?
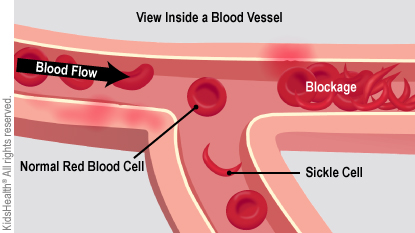
Healthy red blood cells are soft, flexible, and round. Sickle cell disease makes red blood cells become sticky, hard, and C-shaped. The sickle cells get stuck and block the blood flowing inside small blood vessels. This can be painful and lead to other problems that need to be treated in a hospital.
Sickle cells also break down more quickly than healthy red blood cells. Not having enough red blood cells can lead to anemia. People with anemia feel tired and have less energy.
How Does Hydroxyurea Help People With Sickle Cell Disease?
Hydroxyurea (pronounced: hy-drok-see-yer-EE-uh) helps the body make a type of hemoglobin that helps keep red blood cells round. Hemoglobin is the protein inside red blood cells that carries oxygen to the body. Round and flexible red blood cells work better and last longer. So people who take hydroxyurea can have more energy, and less pain and anemia. They often spend less time in the hospital.
Who Can Take Hydroxyurea?
People who are 9 months and older can take hydroxyurea. A doctor may recommend it if a person has a certain type of sickle cell disease, or based on their symptoms.
You may have heard about hydroxyurea being used to treat other kinds of health problems, not just sickle cell disease. Like many medicines, hydroxyurea has different uses. In very high doses, it can help with some kinds of blood cancers. The dose used to treat sickle cell disease is very low.
What's It Like to Take Hydroxyurea?
Here are the basics of taking hydroxyurea:
- Type of medicine: It’s a liquid medicine or a small capsule.
- Dose: You swallow it one time each day.
- Timing: You take it at the same time every day. (Some people like to set a reminder on their phone.)
You get one blood test before you start the medicine. Then blood tests are done monthly or less often.
Does Hydroxyurea Cause Side Effects?
Most people who take hydroxyurea do well and don’t notice any side effects. Those who do might have decreased white blood cells. Rarely, someone might have dark fingernails or headaches. Often, side effects go away quickly as a person adjusts to the new medicine. If you have side effects, the doctor can change your dose or stop the medicine.
How Much Does Hydroxyurea Cost?
Hydroxyurea is usually paid for by insurance. Your cost (if any) will depend on the type of insurance you have. Your doctor’s office will help you find out if there are costs for you.
If your care team recommends hydroxyurea, talk to them about it. Ask questions and share any concerns. Talk it over with a parent or an adult you trust. Soon you’ll be ready to make a choice you can feel good about.


